In recent years, the devastating impact of the fentanyl crisis has been felt by many Americans. The opioid epidemic, led by this potent synthetic drug, has claimed thousands of lives and shows no signs of abating. But now, a new threat lurks in the shadows, poised to exacerbate an already dire situation — a veterinary sedative known as xylazine.
First synthesized in the 1960s, xylazine is a non-opioid sedative, analgesic, and muscle relaxant used primarily in veterinary medicine for large animals such as horses1. However, it has started to creep into illicit drug markets, often used as an adulterant for opioids like heroin and fentanyl2. The rise of this trend is concerning, and it’s crucial to shed light on this development as it continues to evolve.

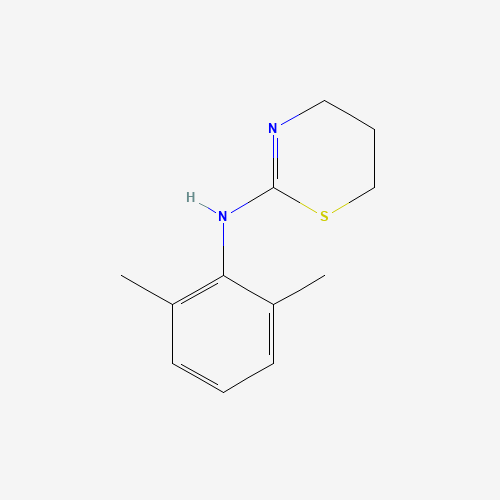
Xylazine, when used in humans, can induce effects similar to those of opioids — a deep sense of relaxation, sedation, and pain relief1. This might explain its allure for those entrenched in substance misuse, but these effects come at a steep price. Unlike traditional opioids, xylazine is not reversed by naloxone (Narcan), the standard emergency treatment for opioid overdoses3. This significantly complicates matters for first responders, who may be unaware that xylazine is present and find that their typical lifesaving interventions are ineffective.
Moreover, xylazine possesses several harmful side effects, including hypotension, bradycardia, respiratory depression, and, in some cases, even death4. Coupled with fentanyl — a substance already notorious for its fatal potency — the presence of xylazine is a ticking time bomb.
The issue of xylazine adulteration in the opioid supply is gaining recognition, yet its severity remains underestimated. According to a 2023 report in the New England Journal of Medicine, xylazine was found in more than 90% of illicit drug samples tested in Philadelphia in 20215. The report found that xylazine is typically found as an adulterant in polydrug mixtures, usually containing simulants like cocaine and amphetamines or opioids like heroin or fentanyl. Alarmingly, the report estimates that the number of xylazine-involved drug-poisoning deaths in the United States increased by 13 times from 2018 to 2021 (an increase from 250 to 3500 deaths).
This rapidly growing and evolving crisis calls for a broad, multi-faceted response involving policymakers, healthcare providers, researchers, and communities. Actions include tightening regulation of veterinary substances, amplifying harm reduction services, and research and development of new overdose drugs that work against xylazine.
The already formidable challenge of the fentanyl and opioid crises is deepened by the introduction of xylazine, adding another lethal layer to the issue. To protect those grappling with substance misuse, it’s crucial to adapt our strategies to this emerging reality. Through a combination of awareness, education, vigilance, and research, we can start to tackle the profound impact of xylazine on the opioid crisis.
References
- Ruiz-Colón, K.; Chavez-Arias, C.; Díaz-Alcalá, J. E.; Martínez, M. A. Xylazine Intoxication in Humans and Its Importance as an Emerging Adulterant in Abused Drugs: A Comprehensive Review of the Literature. Forensic Sci. Int. 2014, 240, 1–8. https://doi.org/10.1016/j.forsciint.2014.03.015.
- Kacinko, S. L.; Mohr, A. L. A.; Logan, B. K.; Barbieri, E. J. Xylazine: Pharmacology Review and Prevalence and Drug Combinations in Forensic Toxicology Casework. J. Anal. Toxicol. 2022, 46 (8), 911–917. https://doi.org/10.1093/jat/bkac049.
- National Institute on Drug Abuse. Xylazine. National Institutes of Health. https://nida.nih.gov/research-topics/xylazine (accessed 2023-05-25).
- Andrew McAward. Xylazine, an Emerging Adulterant. American College of Emergency Physicians. https://www.acep.org/talem/newsroom/oct-2021/xylazine-an-emerging-adulterant (accessed 2023-05-25).
- Gupta, R.; Holtgrave, D. R.; Ashburn, M. A. Xylazine — Medical and Public Health Imperatives. N. Engl. J. Med. 2023, 0 (0), null. https://doi.org/10.1056/NEJMp2303120.